Even slight elevations in iodine intake may produce higher levels of TPOAb in pregnant women (Sun et al., 2022; Shi et al., 2016; Habimana et al., 2014).
Maternal TPOAb positivity is associated with lower IQ in the offspring (Derakhshan et al., 2018; Wasserman et al., 2012), ADHD and behavioral problems (Ghassabian et al., 2012; 2011), as well as miscarriage and preterm delivery (Consortium on Thyroid and Pregnancy-Study Group on Preterm Birth, 2019; Thangaratinam et al., 2012; He et al., 2012). It is also tied to autism (Wang et al., 2025; Brown et al., 2015).
Evidence obtained from the Baltimore Collaborative Perinatal Project showed that maternal TPOAb positivity was associated with lower IQ in children at 4 years of age - same age as the MIREC children in Canada (Wasserman et al. 2012).
Elevated TPOAb values in pregnancy are related to elevated TSH and FT4 levels (Wang et al., 2014). [See this mirrored in the MIREC data - (Hall et al., 2023).]
2. ADHD and Iodine Intake/Thyroid Dysfunction
The studies below document the association of ADHD with maternal iodine supplementation and/or thyroid dysfunction/autoimmunity.
Abel MH, Ystrom E, Caspersen IH, Meltzer HM, Aase H, Torheim LE, Askeland RB, Reichborn-Kjennerud T, Brantsæter AL - "Maternal Iodine Intake and Offspring Attention-Deficit/Hyperactivity Disorder: Results from a Large Prospective Cohort Study" Nutrients 9(11):1239 (2017) doi: 10.3390/nu9111239 MoBa
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5707711/
"The maternal use of supplemental iodine was associated with an increased risk of child ADHD diagnosis and a higher mean ADHD symptom score...Initiating iodine supplement use in the first trimester was associated with an increased risk of ADHD diagnosis, whereas use before pregnancy was associated with increased child ADHD symptom scores."
Engel SM, Villanger GD, Herring A, Nethery RC, Drover SSM, Zoeller RT, Meltzer HM, Zeiner P, Knudsen GP, Reichborn-Kjennerud T, Longnecker MP, Aase H - "Gestational thyroid hormone concentrations and risk of attention-deficit hyperactivity disorder in the Norwegian Mother, Father and Child Cohort Study" Paediatr Perinat Epidemiol 37(3):218-228 (2023) doi: 10.1111/ppe.12941
https://onlinelibrary.wiley.com/doi/10.1111/ppe.12941. MoBa
"Both high and low concentrations of maternal thyroid hormones, although within population reference ranges, increase the risk of ADHD in offspring."
Endendijk JJ, Wijnen HAA, Pop VJM, van Baar AL - "Maternal thyroid hormone trajectories during pregnancy and child behavioral problems" Horm Behav 94:84-92 (2017). doi: 10.1016/j.yhbeh.2017.06.007
https://www.sciencedirect.com/science/a ... 6X17300156
"The course of maternal thyroid levels during pregnancy is important for child behavior problems. Mothers with flattened T4 and TSH curves during pregnancy have children with highest anxiety/depression symptoms. Boys are more vulnerable than girls to develop attention problems in response to high first-trimester maternal TSH levels."
Feng Y, Li J, Lok KYW, Chau PH, Lu D, Kwok JYY - "Maternal thyroid dysfunction and stress during pregnancy on ADHD risk in preschoolers: a retrospective study" Eur Child Adolesc Psychiatry. 2025 Jun 23. doi: 10.1007/s00787-025-02792-9
https://link.springer.com/article/10.10 ... 25-02792-9
"In the adjusted model, children of mothers with thyroid dysfunction during pregnancy had a 54.1% higher risk of an ADHD diagnosis (95% CI: 1.050, 2.262) compared to those whose mothers did not have thyroid dysfunction."
Ge GM, Leung MTY, Man KKC, Leung WC, Ip P, Li GHY, Wong ICK, Kung AWC, Cheung CL - "Maternal Thyroid Dysfunction During Pregnancy and the Risk of Adverse Outcomes in the Offspring: A Systematic Review and Meta-Analysis" J Clin Endocrinol Metab 105(12):dgaa555 (2020) doi: 10.1210/clinem/dgaa555
https://academic.oup.com/jcem/article/1 ... 21/5893988
"We identified 29 eligible articles and found an association between maternal hyperthyroidism and attention deficit hyperactivity disorder (ADHD) (OR: 1.18, 95% CI: 1.04-1.34, I2 = 0%) and epilepsy (OR: 1.19, 95% CI: 1.08-1.31, I2 = 0%) in offspring; as well as an association of maternal hypothyroidism with increased risk of ADHD (OR: 1.14, 95% CI: 1.03-1.26, I2 = 25%), autism spectrum disorder (OR: 1.41, 95% CI: 1.05-1.90, I2 = 63%), and epilepsy (OR: 1.21, 95% CI: 1.06-1.39, I2 = 0%) in offspring."
Ghassabian A, Bongers-Schokking JJ, de Rijke YB, van Mil N, Jaddoe VW, de Muinck Keizer-Schrama SM, Hooijkaas H, Hofman A, Visser W, Roman GC, Visser TJ, Verhulst FC, Tiemeier H - "Maternal thyroid autoimmunity during pregnancy and the risk of attention deficit/hyperactivity problems in children: the Generation R Study" Thyroid 22(2):178-86 (2012). doi: 10.1089/thy.2011.0318
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3271370/ Generation R
"However, elevated titers of TPOAbs in mothers were associated with externalizing problems in children (odds ratio [OR]=1.64, 95% confidence interval [CI]: 1.17–2.29, p=0.004). In particular, children of TPOAb-positive mothers were at a higher risk of attention deficit/hyperactivity problems (OR=1.77, 95% CI: 1.15–2.72, p=0.01)."
Komendová I, Špitálníková S - "Intellectual performance of children of mothers with an untreated thyroid disorder in the first trimester of pregnancy" Endokrynol Pol 69(3):241-245 (2018) doi: 10.5603/EP.a2018.0025
https://journals.viamedica.pl/endokryno ... view/55883
"The experimental group did exhibit a statistically significant increase in the percentage of children with a suspected SLD or clinically significant attention issues (p =0.05)... Conclusion: Untreated thyroid disorders in the first trimester of pregnancy can increase the risk of the child developing attention or learning issues."
Modesto T, Tiemeier H, Peeters RP, Jaddoe VW, Hofman A, Verhulst FC, Ghassabian A - "Maternal Mild Thyroid Hormone Insufficiency in Early Pregnancy and Attention-Deficit/Hyperactivity Disorder Symptoms in Children" JAMA Pediatr 169(9):838-45 (2015) doi: 10.1001/jamapediatrics.2015.0498 Generation R
https://jamanetwork.com/journals/jamape ... le/2344550
"Children exposed to maternal hypothyroxinemia in early pregnancy had more ADHD symptoms, independent of confounders."
Nielsen TC, Nassar N, Shand AW, Jones H, Guastella AJ, Dale RC, Lain SJ - "Association of Maternal Autoimmune Disease With Attention-Deficit/Hyperactivity Disorder in Children" JAMA Pediatr 175(3):e205487 (2021). doi: 10.1001/jamapediatrics.2020.5487
In this cohort study, maternal autoimmune diseases were associated with increased ADHD among children.
Päkkilä F, Männistö T, Pouta A, Hartikainen AL, Ruokonen A, Surcel HM, Bloigu A, Vääräsmäki M, Järvelin MR, Moilanen I, Suvanto E - "The impact of gestational thyroid hormone concentrations on ADHD symptoms of the child" J Clin Endocrinol Metab 99(1):E1-8 (2014) doi: 10.1210/jc.2013-2943.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3879664/
This study demonstrated a statistically significant but modest link between increasing maternal TSH levels in early pregnancy and teacher-rated ADHD symptoms in female offspring at age 8. Girls had a 1.2-fold odds of inattention and Rutter scores of 9 or greater and 1.4-fold odds of combined ADHD symptoms with every natural log increase in maternal TSH.
Sepehrmanesh Z, Moraveji A, Ahmadvand A, Mehri Z - "The Duration of Breastfeeding and Attention-Deficit Hyperactivity Disorder in School-Aged Children" Comprehensive Child and Adolescent Nursing 45(1):22-30 (2020)
https://doi.org/10.1080/24694193.2020.1797236
- Also SEE: SSRIs and Autism:
Holland L, Drummond K, Thomson S, Sominsky L, Marx W, Love C, Dawson SL, Harrison LC, Saffery R, Symeonides C, Tang ML, Burgner D, Sly PD, Vuillermin P, Ponsonby AL; BIS Investigator group; Mansell T, Ranganathan S, O'Hely M - "Prenatal and birth factors associated with child autism diagnosis: a birth cohort perspective" Pediatr Res. 2026 Jan 15. doi: 10.1038/s41390-025-04747-x
https://www.nature.com/articles/s41390-025-04747-x
https://academic.oup.com/jcem/article-a ... 54/2844344
"Over a period of almost 10 yr, we carried out a prospective study of the neuropsychological development of the offspring of 16 women from a moderately iodine-deficient area (area A) and of 11 control women from a marginally iodine-sufficient area (area B) whose thyroid function had been monitored during early gestation...Attention deficit and hyperactivity disorder (ADHD) was diagnosed in 11 of 16 area A children (68.7%) but in none from area B."
Villanger GD, Ystrom E, Engel SM, Longnecker MP, Pettersen R, Rowe AD, Reichborn-Kjennerud T, Aase H - "Neonatal thyroid-stimulating hormone and association with attention-deficit/hyperactivity disorder" Paediatr Perinat Epidemiol 34(5):590-596 (2020) doi: 10.1111/ppe.12643
https://onlinelibrary.wiley.com/doi/10.1111/ppe.12643. MoBa
"In multivariable, quintile models the relationship appeared to follow a U-shaped pattern with elevated odds ratios (OR) at lower and higher TSH levels."
- see: Alvarez-Pedrerol M, Ribas-Fitó N, Torrent M, Julvez J, Ferrer C, Sunyer J - "TSH concentration within the normal range is associated with cognitive function and ADHD symptoms in healthy preschoolers" Clin Endocrinol (Oxf) 66(6):890-8 (2007)
https://onlinelibrary.wiley.com/doi/10. ... 07.02871.x
Pérez-Lobato R, Ramos R, Arrebola JP, Calvente I, Ocón-Hernández O, Dávila-Arias C, Pérez-García M, Olea N, Fernández MF - "Thyroid status and its association with cognitive functioning in healthy boys at 10 years of age" Eur J Endocrinol 172(2):129-39 (2015)
https://eje.bioscientifica.com/view/jou ... /2/129.xml
"Thus, poor child cognitive function is significantly associated with higher TSH levels but not with intermediate levels, following an inverse U-shaped curve."
The following studies report on the association of Thyroid Peroxidase Antibodies (TPOAb) with increased iodine intake, and the association of elevated TPOab with loss of IQ and ADHD.
Brown AS, Surcel HM, Hinkka-Yli-Salomäki S, Cheslack-Postava K, Bao Y, Sourander A - "Maternal thyroid autoantibody and elevated risk of autism in a national birth cohort" Prog Neuropsychopharmacol Biol Psychiatry 57:86-92 (2015) doi: 10.1016/j.pnpbp.2014.10.010
https://linkinghub.elsevier.com/retriev ... 14)00201-2
"Results: The prevalence of maternal TPO-Ab+ was significantly increased in pregnancies giving rise to autism cases (6.15%) compared to controls (3.54%). The odds of autism were increased by nearly 80% among offspring of mothers who were TPO-Ab+ during pregnancy (OR=1.78, 95% CI=1.16-2.75, p=0.009), compared to mothers negative for this autoantibody. There was also a significant relationship between maternal TPO-Ab defined as a continuous variable and odds of autism (OR=1.09, 95% CI=1.01, 1.17, p=0.02)."
Chen D, Meng F, Liu L, Du Y, Jiao L, Liu S, Liu Y, Huang J, Wang X, Liang N, Sun G, Xi J - "A typical investigation of thyroid nodules in adults of Juye county of Shandong province" Chinese Journal of Control of Endemic Diseases 29(1):5-8 (2014)
https://www.cabdirect.org/globalhealth/ ... 0143211874
Consortium on Thyroid and Pregnancy—Study Group on Preterm Birth; Korevaar TIM, Derakhshan A, Taylor PN, Meima M, Chen L, Bliddal S, Carty DM, Meems M, Vaidya B, Shields B, Ghafoor F, Popova PV, Mosso L, Oken E, Suvanto E, Hisada A, Yoshinaga J, Brown SJ, Bassols J, Auvinen J, Bramer WM, López-Bermejo A, Dayan C, Boucai L, Vafeiadi M, Grineva EN, Tkachuck AS, Pop VJM, Vrijkotte TG, Guxens M, Chatzi L, Sunyer J, Jiménez-Zabala A, Riaño I, Murcia M, Lu X, Mukhtar S, Delles C, Feldt-Rasmussen U, Nelson SM, Alexander EK, Chaker L, Männistö T, Walsh JP, Pearce EN, Steegers EAP, Peeters RP - "Association of Thyroid Function Test Abnormalities and Thyroid Autoimmunity With Preterm Birth: A Systematic Review and Meta-analysis" JAMA 322(7):632-641 (2019) doi: 10.1001/jama.2019.10931
https://jamanetwork.com/journals/jama/f ... le/2748509
Derakhshan A, Korevaar TIM, Taylor PN, Levie D, Guxens M, Jaddoe VWV, Nelson SM, Tiemeier H, Peeters RP - "The Association of Maternal Thyroid Autoimmunity During Pregnancy With Child IQ" J Clin Endocrinol Metab 103(10):3729-3736 (2018)
https://pubmed.ncbi.nlm.nih.gov/30020468/
Ghassabian A, Bongers-Schokking JJ, de Rijke YB, van Mil N, Jaddoe VW, de Muinck Keizer-Schrama SM, Hooijkaas H, Hofman A, Visser W, Roman GC, Visser TJ, Verhulst FC, Tiemeier H - "Maternal thyroid autoimmunity during pregnancy and the risk of attention deficit/hyperactivity problems in children: the Generation R Study" Thyroid 22(2):178-86 (2012). doi: 10.1089/thy.2011.0318
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3271370/
Ghassabian A, Bongers-Schokking JJ, Henrichs J, Jaddoe VW, Visser TJ, Visser W, de Muinck Keizer-Schrama SM, Hooijkaas H, Steegers EA, Hofman A, Verhulst FC, van der Ende J, de Rijke YB, Tiemeier H - "Maternal thyroid function during pregnancy and behavioral problems in the offspring: the generation R study" Pediatr Res 69(5 Pt 1):454-9 (2011) doi: 10.1203/PDR.0b013e3182125b0c
https://www.nature.com/articles/pr9201184
Habimana L, Twite KE, Daumerie C, Wallemacq P, Donnen P, Kalenga MK, Robert A - "High prevalence of thyroid dysfunction among pregnant women in Lubumbashi, Democratic Republic of Congo" Thyroid 24(3):568-75 (2014)
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3949433/
He X, Wang P, Wang Z, He X, Xu D, Wang B - "Thyroid antibodies and risk of preterm delivery: a meta-analysis of prospective cohort studies" Eur J Endocrinol 167:455–464 (2012)
Levie D, Derakhshan A, Shu H, Broeren MAC, de Poortere RA, Peeters RP, Bornehag CG, Demeneix B, Korevaar TIM - "The Association of Maternal Iodine Status in Early Pregnancy with Thyroid Function in the Swedish Environmental Longitudinal, Mother and Child, Asthma and Allergy Study" Thyroid 29(11):1660-1668 (2019) doi: 10.1089/thy.2019.0164
https://pubmed.ncbi.nlm.nih.gov/31524090/
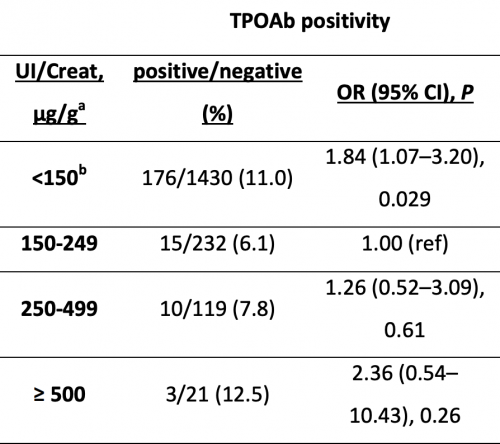
(Note U-shape > iodine deficiency/iodine excess)
Shi X, Han C, Li C, Mao J, Wang W, Xie X, Li C, Xu B, Meng T, Du J, Zhang S, Gao Z, Zhang X, Fan C, Shan Z, Teng W - "Optimal and safe upper limits of iodine intake for early pregnancy in iodine-sufficient regions: a cross-sectional study of 7190 pregnant women in China" J Clin Endocrinol Metab 100(4):1630-8 (2015)
https://pubmed.ncbi.nlm.nih.gov/25629356/
Sun R, Qian TT, Liu LC, Zhao M, Che WJ, Zhang L, Li WD, Jia QZ, Wang JH, Li JS, Chen ZH, Liu P - "Effect of Iodine Supplementation on Iodine Nutrition and Thyroid Function in Pregnant Women: A Cross-Sectional Study" Biomedicine and Environmental Science: English Edition" 7:641-647 (2022)
https://www.besjournal.com/en/article/d ... es2022.083
Thangaratinam S, Tan A, Knox E, Kilby MD, Franklyn J, Coomarasamy A - "Association between thyroid autoantibodies and miscarriage and preterm birth: meta-analysis of evidence" BMJ 342:d2616 (2011) doi: 10.1136/bmj.d2616
https://www.bmj.com/content/342/bmj.d2616.long
Teti C, Panciroli M, Nazzari E, Pesce G, Mariotti S, Olivieri A, Bagnasco M - "Iodoprophylaxis and thyroid autoimmunity: an update" Immunol Res 69(2):129-138 (2021) doi: 10.1007/s12026-021-09192-6
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8106604/
Villanger GD, Ystrom E, Engel SM, Longnecker MP, Pettersen R, Rowe AD, Reichborn-Kjennerud T, Aase H - "Neonatal thyroid-stimulating hormone and association with attention-deficit/hyperactivity disorder" Paediatr Perinat Epidemiol 34(5):590-596 (2020) doi: 10.1111/ppe.12643
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7431377/
Wang X, Jia F, Tian J, Liu D - "Iodine nutrition and thyroid autoantibodies in pregnancy and their relation to thyroid function" Chinese Journal of Endocrinology and Metabolism 5:408-410 (2014)
http://222.198.130.40:81/Qikan/Article/ ... d=49757638
Wang H, Huang K, Piao L, Xue X - "Dysregulation of Thyroid, Growth, and Appetite Hormones in Children and Adolescents With Neurodevelopmental Disorders: A Meta-analysis" J Integr Neurosci 24(10):39816 (2025)
https://doi.org/10.31083/JIN39816
"These changes were mainly observed in ADHD patients, with TPO-Ab increased only in ASD patients."
Wasserman EE, Pillion JP, Duggan A, Nelson K, Rohde C, Seaberg EC, Talor MV, Yolken RH, Rose NR - "Childhood IQ, hearing loss, and maternal thyroid autoimmunity in the Baltimore Collaborative Perinatal Project" Pediatr Res 72(5):525-30 (2012) doi: 10.1038/pr.2012.117
https://www.nature.com/articles/pr2012117
Wu P, Yang M, Teng Y, Ouyang J, Cai W, Tong J, Gao G, Wu X, Han Y, Yan S, Tao F, Huang K - "Association of maternal thyroid peroxidase antibody exposure with children's emotional and behavioral problems" Eur Thyroid J 14(2):e240302 (2025). doi: 10.1530/ETJ-24-0302
https://etj.bioscientifica.com/view/jou ... 4-0302.xml
"After adjusting for potential confounders, maternal TPOAb positivity during the third trimester of pregnancy was found to be associated with an elevated risk of conduct problems in girls, with an odds ratio (OR) of 2.190 (95% confidence interval (CI): 1.137–4.219). Conversely, maternal TPOAb positivity in the first trimester was linked to a decreased incidence of prosocial behavior in boys, with an OR of 0.451 (95% CI: 0.237–0.861). Conclusions Maternal TPOAb positivity during pregnancy may be associated with emotional and behavioral problems in preschool-aged children."
Zhu L, Teng Y, Guo Y, Ru X, Wu X, Hao J, Tao F, Huang K - "Thyroid function test abnormalities-isolated TPOAb+, SCH and hypothyroxinemia and preschool children's neurodevelopment" Clin Endocrinol (Oxf) 99(5):492-501 (2023) doi: 10.1111/cen.14963
https://onlinelibrary.wiley.com/doi/abs ... /cen.14963 (3-6 yearsof age)
"After adjusting for potential confounders in Poisson regression analyses, it showed that maternal isolated TPOAb positivity before 20 gestational weeks may be associated with the increased risk of abnormalities in peer problems (odds ratio [OR] = 1.90, 95% confidence interval [CI]: 1.26, 287). Maternal isolated SCH before 20 gestational weeks was observed to be related with increased risk of abnormalities in inhibition (OR = 2.73, 95% CI: 1.37, 5.41), working memory (OR = 1.67, 95% CI: 1.04, 2.70), conduct problems (OR = 1.80, 95% CI: 1.05, 3.09), hyperactivity (OR = 1.94, 95% CI:1.08, 3.49) and total difficulties (OR = 1.94, 95% CI: 1.13, 3.34). Maternal isolated hypothyroxinemia before 20 gestational was observed to be related with increased risk of abnormalities in peer problems (OR = 2.71, 95% CI: 1.17, 6.27)." NOTE: TPOAb positivity alone seems to increase behavioral vulnerability, consistent with the idea that autoimmunity itself (even without hormone changes) can impact fetal brain development via inflammatory pathways.
=====
Update: July 19, 2023
At low doses, fluoride's anti-iodine properties could potentially offer advantages in certain cases of ADHD stemming from excessive iodine levels. A recent investigation conducted in Gipuzkoa, where nearly all pregnant women were taking a specific iodine supplement - not a multi-vitamin - revealed that elevated levels of maternal urinary fluoride were linked to a reduced risk of cognitive issues, particularly inattention, by the age of 11 (Ibarluzea et al., 2023). Regrettably, the study authors did not provide information regarding iodine intake or factor it into their analysis.
Ibarluzea J, Subiza-Pérez M, Arregi A, Molinuevo A, Arranz-Freijo E, de Miguel MS, Jiménez A, Andiarena A, Santa-Marina L, Lertxundi A - "Association of maternal prenatal urinary fluoride levels with ADHD symptoms in childhood" Environ Res. 2023 Jul 19:116705. doi: 10.1016/j.envres.2023.116705. Epub ahead of print. INMA
https://www.sciencedirect.com/science/a ... 5123015098}
"Higher levels of MUFcr in pregnant women were associated with a lower risk of cognitive problems-inattention at 11 years. These findings are inconsistent with those from previous studies and indicate the need for other population-based studies to confirm or overturn these results."
Studies have also shown that fluoride may reduce TPOab levels in populations with high iodine intake (Chen et al., 2014). Maternal TPOab positivity is associated with increased ADHD in offspring (see above).
Chen Diqun, Meng Fangang, Liu Lixiang, Zhao Rencheng, Du Yang, Jiao Lisha, Liu Shoujun, Liu Yuan, Huang Jumei, Wang Xin, Liang Na, Sun Guodong, Xi Jianguo - "A Typical Survey on Thyroid Nodules in Adults in Juye County, Shandong Province, China" Chin J Ctrl Endem Dis 29(1):5-8 (2014) PFPC Library
"Within the water iodine range of 200–300 μg/L, an increase in water fluoride from (0.99±0.29) mg/L to (1.67±0.19) mg/L led to a significant decrease in both thyroid nodule detection rates and TPOAb positivity rates."
SEE many other studies implicating the effects of iodine on neurodevelopment: viewtopic.php?f=97&t=5022
Other studies of interest:
Yadav R, Goyal M, Aggarwal A, Kulshreshtha B - "Thyroid hormone resistance due to a novel mutation in thyroid hormone receptor presenting as attention deficit hyperactivity disorder" Natl Med J India 37(6):332-334 (2024) doi: 10.25259/NMJI_869_2022
https://pubmed.ncbi.nlm.nih.gov/40257157/
"We report a 21-year-old man with long-standing attention deficit hyperactivity disorder (ADHD) and learning disabilities. His thyroid function tests showed an increased free T3 and T4 in the presence of a non-suppressed TSH. Other pituitary hormones were normal. Subsequently, a genetic analysis revealed a heterozygous mutation (Pro452Thr) in THRβ gene, establishing the diagnosis of RTH. Thus, this was a RTH presenting as ADHD due to a novel mutation in the thyroid hormone receptor gene."
====
SEE ALSO:
Russart KLG, Huk D, Nelson RJ, Kirschner LS - "Elevated aggressive behavior in male mice with thyroid-specific Prkar1a and global Epac1 gene deletion" Horm Behav 98:121-129 (2018) doi: 10.1016/j.yhbeh.2017.12.012
https://pubmed.ncbi.nlm.nih.gov/29289659/
"Although hyperthyroidism has not been previously associated with aggression, increased thyroid hormone signaling might contribute to the increased aggressive response to the intruder mouse, as well as the increased swimming response. Mice with a genetic background of Tpo-Cre;Prkar1aflox/flox;Epac1-/- are aggressive, and both the thyroid-specific knockout of Prkar1a and global knockout of Epac1 likely contribute to this aggressive behavior. This study supports the hypothesis that altered thyroid signaling and aggressive behavior are linked."
Briassoulis G, Keil MF, Naved B, Liu S, Starost MF, Nesterova M, Gokarn N, Batistatos A, Wu TJ, Stratakis CA - "Studies of mice with cyclic AMP-dependent protein kinase (PKA) defects reveal the critical role of PKA's catalytic subunits in anxiety" Behav Brain Res 307:1-10 (2017) doi: 10.1016/j.bbr.2016.03.001
https://pmc.ncbi.nlm.nih.gov/articles/PMC4853257/
"Alterations of PKA activity induced by haploinsufficiency of its main regulatory or most important catalytic subunits result in anxiety-like behaviors."
NOTE: Cyclic adenosine mono-phosphate-dependent protein kinase (PKA) is another way of describing protein kinase C (PKC), which is activated downstream of the Gq/11 signaling pathway.
Ugolini M, Keil MF, Paradiso E, Wu J, Stratakis CA - "Anxiety-like behavior and other consequences of early life stress in mice with increased protein kinase A activity" Behav Brain Res 348:22-30 (2018) doi: 10.1016/j.bbr.2018.04.001
https://pmc.ncbi.nlm.nih.gov/articles/PMC5993604/
"The finding of behavioral differences that are apparent during adolescence in Prkar1a+/- mice suggests that long-term exposure of the brain to increased PKA activity during critical developmental periods contributes to the anxiety-like phenotype noted in the adult animals with increased PKA activity."
Keil MF, Briassoulis G, Gokarn N, Nesterova M, Wu TJ, Stratakis CA - "Anxiety phenotype in mice that overexpress protein kinase A" Psychoneuroendocrinology 37(6):836-43 (2012) doi: 10.1016/j.psyneuen.2011.09.016
https://pmc.ncbi.nlm.nih.gov/articles/PMC3320692/
SEE also:"The role of cyclic adenosine monophosphate/protein kinase A (cAMP/PKA) signaling in the molecular pathways involved in fear and memory is well established. Prior studies in our lab reported that transgenic mice with an inactivating mutation in Prkar1a gene (codes for the 1-alpha regulatory subunit (R1α) of PKA) exhibited behavioral abnormalities including anxiety and depression. In the present study, we examined the role of altered PKA signaling on anxiety-like behaviors in Prkar1a(+/-) mice compared to wild-type (WT) littermates. The elevated plus maze (EPM) and marble bury (MB) tests were used to assess anxiety-like behavior. The hotplate test was performed to evaluate analgesia. We further examined the impact of the Prkar1a inactivating mutation on PKA activity in specific nuclei of the brain associated with anxiety-like behavior. Results for the MB test showed a genotype effect, with increased anxiety-like behavior in Prkar1a(+/-) mice, compared to WT littermates (p<0.05). MANOVA analysis showed a significant genotype difference in anxiety-like behavior in the EPM between WT and Prkar1a(+/-) mice on combined dependent variables (open arm time and open to total time ratio; p<0.05). Results of hotplate testing showed no genotype effect however; the expected sex difference was noted. Analysis of PKA activity showed the loss of one Prkar1a allele led to an increase in basal and cAMP-stimulated kinase activity in both the basolateral and central amygdala. These results suggest that the alteration in PKA signaling in Prkar1a(+/-) mice is not a ubiquitous effect; and supports the importance of cAMP/PKA pathway in neurobiological processes involved in anxiety and fear sensitization."
ADHD - Thyroid - PFAS - Inverse U - Reference Set III
viewtopic.php?f=7&t=5155
ADHD & Fluoride | ADHD & Thyroid
viewtopic.php?f=30&t=4874