Kampouri M, Gustin K, Stråvik M, Barman M, Levi M, Daraki V, Jacobsson B, Sandin A, Sandberg AS, Wold AE, Vahter M, Kippler M - "Association of maternal urinary fluoride concentrations during pregnancy with size at birth and the potential mediation effect by maternal thyroid hormones: The Swedish NICE birth cohort" Environmental Research Available online 20 August 2022, 114129
https://www.sciencedirect.com/science/a ... ihub#bib52
Abstract
Background
Observational studies have indicated that elevated maternal fluoride exposure during pregnancy may impair child neurodevelopment but a potential impact on birth outcomes is understudied.
Objectives
To evaluate the impact of gestational fluoride exposure on birth outcomes (birth size and gestational age at birth) and to assess the potential mediating role of maternal thyroid hormones.
Methods
We studied 583 mother-child dyads in the NICE cohort in northern Sweden. Maternal fluoride exposure was assessed by measuring urinary concentrations at late pregnancy (median: 29th gestational week) using an ion selective electrode. Plasma levels of free and total thyroxine (fT4, tT4) and triiodothyronine (fT3, tT3), and thyroid stimulating hormone (TSH) were measured with electrochemiluminescence immunoassays. The infant's weight, length, head circumference, and gestational age at birth were extracted from hospital records.
Results
Median urinary fluoride concentration was 0.71 mg/L (5th-95th percentile 0.31–1.9 mg/L; specific gravity adjusted). In multivariable-adjusted regression models, every 1 mg/L increase of maternal urinary fluoride was associated with a mean increase in birth weight by 84 g (95%CI: 30, 138), length by 0.41 cm (95%CI: 0.18, 0.65), head circumference by 0.3 cm (95%CI: 0.1, 0.4), and with increased odds of being born large for gestational age (OR = 1.39, 95%CI: 1.03, 1.89). Every 1 mg/L increase of maternal urinary fluoride was also associated with a mean increase of the plasma fT3:fT4 ratio (B = 0.007, 95%CI: 0.000, 0.014), but not with the hormones or TSH. In mediation analyses, the maternal fT3:fT4 ratio did not explain the urinary fluoride-birth size relationships.
Discussion
Gestational urinary fluoride concentrations were associated with increased size at birth and even with increased odds of being born large for gestational age. The fluoride-related associations with increased size at birth were not explained by changes in maternal thyroid hormone levels.
2022 - Sweden NICE - Birth weight and fluoride | Thyroid | Commentary
-
admin
- Site Admin
- Posts: 6757
- Joined: Tue Jan 18, 2005 10:25 pm
-
wendy
- Posts: 228
- Joined: Mon Apr 03, 2006 5:51 am
Re: 2022 - Sweden NICE - Birth weight and fluoride | Thyroid
Jan. 31, 2023 - Re-posted from "State of the Mother" forum.
PFPC Comments
The study by Kampouri et al. reported that "gestational urinary fluoride concentrations" were associated with an increase in birth length and increased odds of being born large for gestational age (LGA).
Authors claim that the "fluoride-related associations with increased size at birth were not explained by changes in maternal thyroid hormone levels."
There are numerous concerns with this statement.
1. "Gestational urinary fluoride concentrations"
Thyroid hormones and fluoride levels were tested only once during gestation - and this in late pregnancy, at week 29 (SD: 1.5; range: 24–36). No other time points were available for comparison.
To investigate any association between LAG and maternal thyroid hormone and urinary fluoride concentrations, the study should have focused on the first half of gestation, particularly the first trimester.
It is during this time that the fetus is wholly dependent on the mother's thyroid hormones. Fetal thyroid function does not begin before 12–14 weeks of pregnancy, and even after the onset of fetal thyroid hormone production, the dependency on maternal thyroid function continues for some time (de Escobar, 2004). Maternal thyroid hormones undergo drastic changes throughout gestation.
Fetal growth patterns determining birth weight and length are already apparent in early pregnancy and can be analyzed by weeks 11-14 (Daouk et al., 2011; Papastefanou et al., 2012; Young et al., 2021).
LGA has been associated with maternal hypothyroxinemia during the first half of pregnancy (Li et al., 2022; Zhu et al., 2018; León et al., 2015), while small for gestational age (SAG) is associated with subclinical hypothyroidism, with some reporting a closer association in the other trimesters (Derakhshan et al., 2020).
A previous study in the same cohort (NICE) had found "inverse associations between urinary Cd and the fT4:tT4 and fT3:tT3 ratios, suggesting a relatively higher increase in total hormone levels compared to free levels, with increasing Cd." (Gustin et al., 2021)
No effort was made to adjust for cadmium intake, despite long-standing and well-documented evidence that cadmium and fluoride may act additively and synergistically (PFPC, 2013). (Both substances may cause mottling of teeth, known as "dental fluorosis".)
This omission is even more surprising considering that lead author Kampouri did an earlier study involving cadmium in Greece that found a "negative association of Cd with TSH persisted only when iodine sufficiency was unfavorable." (Margetaki et al., 2021)
In the present study, a similar finding: "...a statistically significant increase in the fT3:fT4 ratio in women with UICs below 150 μg/L that was not evident in women with concentrations equal or above 150 μg/L was found, which may suggest a possible increased vulnerability of women with low iodine intake."
As data on cadmium, and selenium - essential for deiodination -, were available for this cohort, authors should have adjusted for these variables.
3. UIC <150 ug/L vs UIC >150 ug/L
Once again, in this model, all pregnant women with "more-than-adequate" and "excessive" iodine intake were lumped together with the "adequate" group of UIC >150 ug/L.
This is highly inappropriate, as UIC levels of 250 ug/L and above are associated with an increase in subclinical hypothyroidism (Shi et al., 2015).
Fetal growth parameters are negatively affected by UIC <150 and >250 ug/L (i.e. Chen et al., 2018).
Data should have been stratified by WHO classifications:
According to the study protocol, the mothers were asked to be fasting for 8 hours before study visits (Barman et al., 2018).
Research shows that fasting, especially early in the morning, may impact TSH levels (i.e. Nair et al., 2014).
Further adding to the confusion, drinking fluoride-laden water was allowed, as fasting for a blood test always excludes drinking water.
5. Season of Sampling
The study reports on the seasonal variations pertaining to urinary fluoride samples but made no effort to correlate with the seasonal variations of UIC and thyroid hormones (Kuzmenko et al., 2021).
SUMMARY
As reported by Aghaei et al. earlier (2015), this study found an increase in birth length with increasing fluoride intake. Many other previous studies have reported a decrease in birth weight with increasing fluoride intake.
Both iodine deficiency AND excess may affect birth weight and length. Both hypo- and hyperthyroidism are well-established to negatively affect birth outcomes, including LGA (Turunen et al., 2022; Dong et al., 2021).
Thyroid hormone controls fetal growth and development. Maternal thyroid hormones - upon which the fetus is dependent for the first 20 weeks - undergo drastic changes for the entire duration of gestation.
Maternal hypothyroxinemia has been found associated with LGA in numerous investigations (Li et al., 2021; Ovadia et al., 2022), while subclinical hypothyroidism is associated with SAG and lower birth weight (Derakhshan et al., 2020). Fluoride intake has been associated with both conditions.
Abnormal birth weight and length have also long been documented as a result of fluoride poisoning.
Likewise, the literature on the effects of fluoride on thyroid hormone metabolism now encompasses over 700 papers, dating back more than one hundred years. Over 280 studies have been published in the last twenty years alone.
The authors' conclusions that the effects of "gestational urinary fluoride concentrations" on birth length are not associated with thyroid hormones are not justified, as the authors conducted their investigation only late in pregnancy, while the effects would have likely occurred in the first half of gestation. In addition, a lack of knowledge and understanding of the effects of maternal iodine status/thyroid function contributed to a faulty model, resulting in an erroneous statistical evaluation.
PFPC Canada, August 2022
REFERENCES
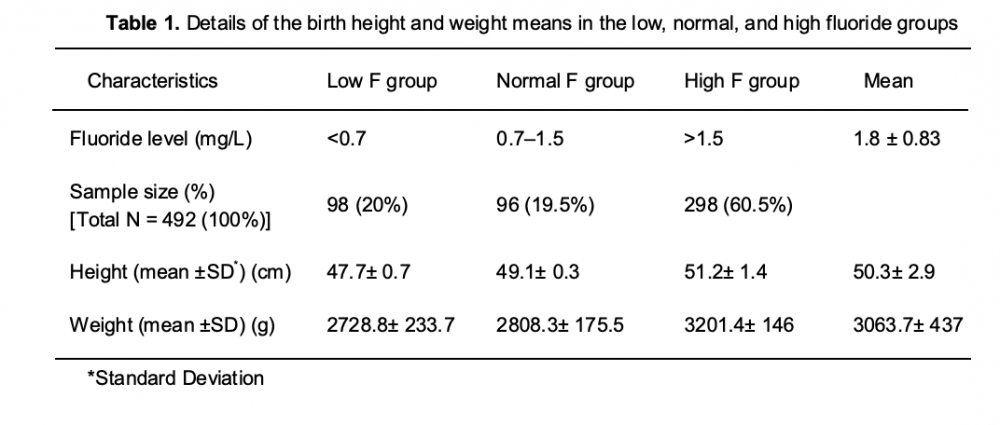
Aghaei M, Derakhshani R, Raoof M, Dehghani M, Mahvi AH - "Effect of fluoride in drinking water on birth height and weight: an ecological study in Kerman Province, Zarand County, Iran" Fluoride 48:160-168 (2015)
https://www.researchgate.net/publicatio ... ounty_Iran
Chen R, Li Q, Cui W, Wang X, Gao Q, Zhong C, Sun G, Chen X, Xiong G, Yang X, Hao L, Yang N - "Maternal Iodine Insufficiency and Excess Are Associated with Adverse Effects on Fetal Growth: A Prospective Cohort Study in Wuhan, China" J Nutr 148(11):1814-1820 (2018)
https://pubmed.ncbi.nlm.nih.gov/30239801/
"The longitudinal analyses showed negative associations of maternal insufficient, more than adequate, or excessive iodine status with fetal growth during pregnancy (all P < 0.05)...Importantly, this study indicated that fetal FL in the second and third trimesters can be adversely affected by insufficient iodine status during early pregnancy."
de Escobar GM, Obregon MJ, del Rey FE - "Iodine deficiency and brain development in the first half of pregnancy" Public Health Nutr 10: 1554–1570 (2004)
Derakhshan A, Peeters RP, Taylor PN, Bliddal S, Carty DM, Meems M, Vaidya B, Chen L, Knight BA, Ghafoor F, Popova PV, Mosso L, Oken E, Suvanto E, Hisada A, Yoshinaga J, Brown SJ, Bassols J, Auvinen J, Bramer WM, López-Bermejo A, Dayan CM, French R, Boucai L, Vafeiadi M, Grineva EN, Pop VJM, Vrijkotte TG, Chatzi L, Sunyer J, Jiménez-Zabala A, Riaño I, Rebagliato M, Lu X, Pirzada A, Männistö T, Delles C, Feldt-Rasmussen U, Alexander EK, Nelson SM, Chaker L, Pearce EN, Guxens M, Steegers EAP, Walsh JP, Korevaar TIM - "Association of maternal thyroid function with birthweight: a systematic review and individual-participant data meta-analysis" Lancet Diabetes Endocrino 8(6):501-510 (2000) doi: 10.1016/S2213-8587(20)30061-9
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8168324/
"Maternal subclinical hypothyroidism in pregnancy is associated with a higher risk of SGA and lower birthweight, whereas isolated hypothyroxinaemia is associated with lower risk of SGA and higher birthweight. There was an inverse, dose-response association of maternal TSH and FT4 (even within the normal range) with birthweight."
Diouf M, Cisse D, Lo CM, Ly M, Faye D, Ndiaye O - "Pregnant women living in areas of endemic fluorosis in Senegal and low birthweight newborns: case-control study" Rev Epidemiol Sante Publique 60(2):103-8 (2012) French. doi: 10.1016/j.respe.2011.09.009
https://pubmed.ncbi.nlm.nih.gov/22424749/
"Low birthweight was associated with pregnant women living in endemic areas."
Dong J, Liu S, Wang L, Zhou X, Zhou Q, Liu C, Zhu J, Yuan W, Xu WY, Deng J - "Iodine monitoring models contribute to avoid adverse birth outcomes related more than adequate iodine intake" BMC Pregnancy Childbirth 21(1):454 (2021)
https://bmcpregnancychildbirth.biomedce ... 21-03936-w
"Multivariate logistic regression analysis showed that multivitamin supplements containing iodine and milk consumption were risk factors for more than adequate iodine (UIC ≥ 250 μg/L). Iodine-rich diet was significantly related to heavier birthweight, larger head circumference and longer femur length of the newborns while more than adequate iodine intake (UIC ≥ 250 μg/L) was a risk factor for macrosomia."
El Daouk M, Langer O, Lysikiewicz A - "First-trimester crown-rump length as a predictor of fetal LGA and SGA at term" J Matern Fetal Neonatal Med. 25(2):162-4 (2012). doi: 10.3109/14767058.2011.566653
"Mean first-trimester CRL of the 63 LGA-term neonates was 62.7 ± 6.0 mm (95% confidence interval, ± 1.49 mm; range, 61.21-64.19), while that of the 58 SGA-term neonates was smaller at 58.8 ± 6.9 mm (95% confidence interval, ± 1.79 mm; range, 57.01-60.59 mm). This 3.9 mm difference between the means was statistically significant (P = 0.01).
Conclusion: We found that birthweights of LGA and SGA neonates at term were associated with their first-trimester CRL measurements, thus, indicating that fetal growth patterns apparent early in pregnancy continue through term."
Gustin K, Barman M, Skröder H, Jacobsson B, Sandin A, Sandberg AS, Wold AE, Vahter M, Kippler M - "Thyroid hormones in relation to toxic metal exposure in pregnancy, and potential interactions with iodine and selenium" Environ Int 157:106869 (2021) doi: 10.1016/j.envint.2021.106869
https://pubmed.ncbi.nlm.nih.gov/34530290/
Gustin K, Barman M, Stråvik M, Levi M, Englund-Ögge L, Murray F, Jacobsson B, Sandberg AS, Sandin A, Wold AE, Vahter M, Kippler M - "Low-level maternal exposure to cadmium, lead, and mercury and birth outcomes in a Swedish prospective birth-cohort" Environ Pollut 265(Pt B):114986 (2020). doi: 10.1016/j.envpol.2020.114986
https://pubmed.ncbi.nlm.nih.gov/32585550/
"In multivariable-adjusted spline regression models, a doubling of maternal erythrocyte Cd (median: 0.29 μg/kg) above the spline knot of 0.50 μg/kg was associated with reduced birth weight (B: -191 g; 95% CI: -315, -68) and length (-0.67 cm; -1.2, -0.14). The association with birth weight remained when the analysis was restricted to never-smokers. Likewise, a doubling of erythrocyte Hg (median 1.5 μg/kg, mainly MeHg) above 1.0 μg/kg, was associated with decreased birth weight (-59 g; -115, -3.0), and length (-0.29 cm; -0.54, -0.047). Maternal Pb (median 11 μg/kg) was unrelated to birth weight and length. Erythrocyte Cd was primarily associated with intake of plant derived foods, Pb with game meat, tea and coffee, and Hg with fish. The results indicated that low-level maternal Cd and Hg exposure were associated with poorer birth anthropometry. Further prospective studies in low-level exposed populations are warranted."
Gustin K, Vahter M, Barman M, Jacobsson B, Skröder H, Filipsson Nyström H, Sandin A, Sandberg AS, Wold AE, Kippler M - "Assessment of Joint Impact of Iodine, Selenium, and Zinc Status on Women's Third-Trimester Plasma Thyroid Hormone Concentrations" J Nutr 152(7):1737-1746 (2022) doi: 10.1093/jn/nxac081
https://pubmed.ncbi.nlm.nih.gov/35383840/
SAME "NICE" COHORT.
"Results: Plasma zinc was most influential for all hormones but tT3, for which plasma selenium was most influential. In adjusted linear regression models, zinc was positively associated with tT4, tT3, and TSH, and <1200 μg/L also with fT4 and fT3. Selenium was inversely associated with fT3, and <85 μg/L with tT3."
Huang D, Zhu H, Zhu Y, Dang Q, Yang Q, Zhang Y, Cai X, Zhao X, Liang N, Wang H, Yu H - "Association of maternal HDL2-c concentration in the first trimester and the risk of large for gestational age birth" Lipids Health Dis 21(1):71 (2022) doi: 10.1186/s12944-022-01688-w.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9380360/
Kuzmenko NV, Tsyrlin VA, Pliss MG, Galagudza MM - "Seasonal variations in levels of human thyroid-stimulating hormone and thyroid hormones: a meta-analysis" Chronobiol Int 38(3):301-317 (2021) doi: 10.1080/07420528.2020.1865394
https://www.tandfonline.com/doi/abs/10. ... ode=icbi20
"We found that circulating TSH levels were higher in winter than in other seasons, and FT4 levels were higher in autumn than in winter. T4 level had no pronounced seasonal dynamics. The level of circulating T3 was significantly higher in winter than in summer and FT3 levels were lower in summer than in autumn and spring. In addition, analysis of TSH seasonal dynamics (winter vs summer) accounting for gender differences showed pronounced increases in TSH levels during winter in women, but not in men; and also significant increases in FT4 levels during summer in men, but not in women."
León G, Murcia M, Rebagliato M, Álvarez-Pedrerol M, Castilla AM, Basterrechea M, Iñiguez C, Fernández-Somoano A, Blarduni E, Foradada CM, Tardón A, Vioque J - "Maternal thyroid dysfunction during gestation, preterm delivery, and birthweight. The Infancia y Medio Ambiente Cohort, Spain" Paediatr Perinat Epidemiol 29(2):113-22 (2015). doi: 10.1111/ppe.12172
https://pubmed.ncbi.nlm.nih.gov/25565408/
"An inverse association of fT4 and TSH with birthweight was found, the former remaining when restricted to euthyroid women. High fT4 levels were also associated with an increased risk of SGA [odds ratio, 95% confidence interval (CI) 1.28 (95% CI 1.08, 1.51)]. Mean birthweight was higher in the hypothyroxinaemic group (β = 109, P < 0.01). Iodine intake and UIC were not associated with birth outcomes."
Li P, Cui J, Li L, Chen X, Ouyang L, Fan J, Lin S - "Association between isolated maternal hypothyroxinemia during the first trimester and adverse pregnancy outcomes in Southern Chinese women: a retrospective study of 7051 cases" BMC Pregnancy Childbirth 22(1):866 (2022) doi: 10.1186/s12884-022-05194-w
https://pubmed.ncbi.nlm.nih.gov/36424562/
"However, after using multivariate logistic regression analysis to adjust for confounders (maternal age, educational levels and preBMI), only LGA was shown to be associated with an increased risk in IMH women [adjusted OR: 1.27 (95% CI 1.044-1.566)]."
Margetaki K, Vafeiadi M, Kampouri M, Roumeliotaki T, Karakosta P, Daraki V, Kogevinas M, Hu H, Kippler M, Chatzi L - "Associations of exposure to cadmium, antimony, lead and their mixture with gestational thyroid homeostasis" Environ Pollut 289:117905 (2021) doi: 10.1016/j.envpol.2021.117905
https://pubmed.ncbi.nlm.nih.gov/34371266/
"In addition, women with high urinary Cd had 2.2 % (95%CI: 0.0 %, 4.4 %) higher fT4 and 4.0 % (95%CI: -0.1 %, 8.1 %) higher fT3 levels, and women with high urinary Pb had 4 % (95%CI: 0.2 %, 8.0 %) higher fT3 levels compared to women with low exposure. The negative association of Cd with TSH persisted only when iodine sufficiency was unfavorable. BKMR attested that simultaneous exposure to toxic metals was associated with decreased TSH and increased fT3 and revealed a potential synergistic interaction of Cd and Pb in association with TSH. The present results suggest that exposure to toxic metals even at low levels can alter gestational thyroid homeostasis."
Männistö T, Vääräsmäki M, Pouta A, Hartikainen AL, Ruokonen A, Surcel HM, Bloigu A, Järvelin MR, Suvanto-Luukkonen E - "Perinatal outcome of children born to mothers with thyroid dysfunction or antibodies: a prospective population-based cohort study" J Clin Endocrinol Metab 94(3):772-9 (2009)doi: 10.1210/jc.2008-1520
https://pubmed.ncbi.nlm.nih.gov/19106271/
"The offspring of TPO-Ab- and TG-Ab-positive mothers had higher perinatal mortality, which was not affected by thyroid hormone status. Unadjusted and adjusted (for maternal age and parity) risk for increased perinatal mortality was an odds ratio of 3.1 (95% confidence interval 1.4-7.1) and 3.2 (1.4-7.1) in TPO-Ab- and 2.6 (1.1-6.2) and 2.5 (1.1-5.9) in TG-Ab-positive mothers. TPO-Ab-positive mothers had more large-for-gestational age infants (2.4 vs. 0.8%, P = 0.017), as did mothers with low TSH and high fT4 concentrations vs. reference group (6.6 vs. 2.5%, P = 0.045). Significantly higher placental weights were observed among mothers with low TSH and high fT4 or high TSH and low fT4 levels as well as among TPO-Ab-positive mothers....Conclusions: First-trimester antibody positivity is a risk factor for perinatal death but not thyroid hormone status as such. Thyroid dysfunction early in pregnancy seems to affect fetal and placental growth."
Medici M, Ghassabian A, Visser W, de Muinck Keizer-Schrama SM, Jaddoe VW, Visser WE, Hooijkaas H, Hofman A, Steegers EA, Bongers-Schokking JJ - "Women with high early pregnancy urinary iodine levels have an increased risk of hyperthyroid newborns: the population-based Generation R Study"
Clin Endocrinol (Oxf) 80:598-606 (2014)
Nair R, Mahadevan S, Muralidharan RS, Madhavan S - "Does fasting or postprandial state affect thyroid function testing?" Indian J Endocrinol Metab. 18(5):705-7 (2014) doi: 10.4103/2230-8210.139237
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4171896/
"TSH was suppressed in all subjects after food irrespective of the fasting levels. Free T4 values did not change significantly. This resulted in reclassification of 15 out of 20 (75%) subjects as subclinical hypothyroidism (SCH) based on fasting values whose TSH values were otherwise within range in the postprandial sample. This may have an impact on the diagnosis and management of hypothyroidism especially where even marginal changes in TSH may be clinically relevant as in SCH and in pregnancy."
Ortíz-García SG, Torres-Sánchez LE, Muñoz-Rocha TV, Mercado-García A, Peterson KE, Hu H, Osorio-Yáñez C, Téllez-Rojo MM - "Maternal urinary fluoride during pregnancy and birth weight and length: Results from ELEMENT cohort study" Sci Total Environ 838(Pt 3):156459 (2022). doi: 10.1016/j.scitotenv.2022.156459
https://www.sciencedirect.com/science/a ... via%3Dihub
Papastefanou I, Souka AP, Pilalis A, Eleftheriades M, Michalitsi V, Kassanos D - "First trimester prediction of small- and large-for-gestation neonates by an integrated model incorporating ultrasound parameters, biochemical indices and maternal characteristics" Acta Obstet Gynecol Scand 91(1):104-111 (2012) doi: 10.1111/j.1600-0412.2011.01271.x
https://pubmed.ncbi.nlm.nih.gov/21895614/
"Prediction for birthweight deviations is feasible using data available at the routine 11-14 weeks' examination."
PFPC - "Cadmiosis = Fluorosis" (2013)
viewtopic.php?f=29&t=680
Stråvik M, Gustin K, Barman M, Skröder H, Sandin A, Wold AE, Sandberg AS, Kippler M, Vahter M - "Infant Iodine and Selenium Status in Relation to Maternal Status and Diet During Pregnancy and Lactation" Front Nutr 8:733602 (2021). doi: 10.3389/fnut.2021.733602. PMID: 34988107; PMCID: PMC8721874.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8721874/
Turunen S, Vääräsmäki M, Marttila R, Leinonen MK, Gissler M, Männistö T, Suvanto E - "Indications for intensive care unit treatment among neonates born to mothers with thyroid disease: A population-based cohort study" Acta Obstet Gynecol Scand 101(10):1093-1101 (2022) doi: 10.1111/aogs.14413
https://pubmed.ncbi.nlm.nih.gov/35778835/
"The preterm neonates, neonates with low birthweight, and large-for-gestational-age infants had increased odds of NICU admission if their mother had hypothyroidism. Also neonates with cardiovascular problems, jaundice or hypoglycemia associated with maternal diabetes had increased odds of NICU admissions if their mother had hypothyroidism. Further, the preterm neonates, large-for-gestational-age infants, and term infants with jaundice had increased odds of NICU admission if their mother had hyperthyroidism."
Young AE, Kemp JF, Uhlson C, Westcott JL, Ali SA, Saleem S, Garcès A, Figueroa L, Somannavar MS, Goudar SS, Hambidge KM, Hendricks AE, Krebs NF; Women First Preconception Maternal Nutrition Trial Group - "Improved first trimester maternal iodine status with preconception supplementation: The Women First Trial" Matern Child Nutr 17(4):e13204 (2021). doi: 10.1111/mcn.13204
"Nominally significant positive associations were observed between I/Cr at 12 weeks and birth length and head circumference z-scores (p = 0.028 and p = 0.005, respectively)."
Zhu YD, Han Y, Huang K, Zhu BB, Yan SQ, Ge X, Zhou SS, Xu YY, Ren LI, Sheng J, Pan WJ, Hao JH, Zhu P, Tao FB - "The impact of isolated maternal hypothyroxinaemia on the incidence of large-for-gestational-age infants: the Ma'anshan Birth Cohort study" BJOG 125(9):1118-1125 (2018) doi: 10.1111/1471-0528.15107
First T: (mean = 10.01 weeks; SD 2.13) 2nd T: (mean = 25.64 weeks; SD 1.07)
"However, an increased risk of LGA was observed among IMH women in the second trimester (OR: 2.088, 95% CI: 1.193-3.654). Maternal TPO-Ab positivity in the second trimester increased the risk of SGA (OR: 2.094, 95% CI: 1.333-3.290)."
PFPC Comments
The study by Kampouri et al. reported that "gestational urinary fluoride concentrations" were associated with an increase in birth length and increased odds of being born large for gestational age (LGA).
Authors claim that the "fluoride-related associations with increased size at birth were not explained by changes in maternal thyroid hormone levels."
There are numerous concerns with this statement.
1. "Gestational urinary fluoride concentrations"
Thyroid hormones and fluoride levels were tested only once during gestation - and this in late pregnancy, at week 29 (SD: 1.5; range: 24–36). No other time points were available for comparison.
To investigate any association between LAG and maternal thyroid hormone and urinary fluoride concentrations, the study should have focused on the first half of gestation, particularly the first trimester.
It is during this time that the fetus is wholly dependent on the mother's thyroid hormones. Fetal thyroid function does not begin before 12–14 weeks of pregnancy, and even after the onset of fetal thyroid hormone production, the dependency on maternal thyroid function continues for some time (de Escobar, 2004). Maternal thyroid hormones undergo drastic changes throughout gestation.
Fetal growth patterns determining birth weight and length are already apparent in early pregnancy and can be analyzed by weeks 11-14 (Daouk et al., 2011; Papastefanou et al., 2012; Young et al., 2021).
LGA has been associated with maternal hypothyroxinemia during the first half of pregnancy (Li et al., 2022; Zhu et al., 2018; León et al., 2015), while small for gestational age (SAG) is associated with subclinical hypothyroidism, with some reporting a closer association in the other trimesters (Derakhshan et al., 2020).
- In this context, it is interesting to note that another recent study on the effects of maternal fluoride intake on birth weight/length found that maternal urinary fluoride levels in the first trimester only were associated with an increase in birth length (Ortíz-García et al., 2022), while a decrease in length was associated with fluoride in the second and third trimesters. Unfortunately, that study from Mexico (ELEMENT) did not account for iodine/thyroid status. Iodine intake has been shown to be much higher than adequate for the majority of children and adults in Mexico. More-than-adequate iodine intake may cause subclinical hypothyroidism - mirroring the effects of iodine deficiency, or fluoride poisoning (PFPC, 2022). More-than-adequate iodine intake from milk and iodine supplements has been associated with macrosomia (LGA) (Dong et al, 2021).
A previous study in the same cohort (NICE) had found "inverse associations between urinary Cd and the fT4:tT4 and fT3:tT3 ratios, suggesting a relatively higher increase in total hormone levels compared to free levels, with increasing Cd." (Gustin et al., 2021)
No effort was made to adjust for cadmium intake, despite long-standing and well-documented evidence that cadmium and fluoride may act additively and synergistically (PFPC, 2013). (Both substances may cause mottling of teeth, known as "dental fluorosis".)
This omission is even more surprising considering that lead author Kampouri did an earlier study involving cadmium in Greece that found a "negative association of Cd with TSH persisted only when iodine sufficiency was unfavorable." (Margetaki et al., 2021)
In the present study, a similar finding: "...a statistically significant increase in the fT3:fT4 ratio in women with UICs below 150 μg/L that was not evident in women with concentrations equal or above 150 μg/L was found, which may suggest a possible increased vulnerability of women with low iodine intake."
As data on cadmium, and selenium - essential for deiodination -, were available for this cohort, authors should have adjusted for these variables.
3. UIC <150 ug/L vs UIC >150 ug/L
Once again, in this model, all pregnant women with "more-than-adequate" and "excessive" iodine intake were lumped together with the "adequate" group of UIC >150 ug/L.
This is highly inappropriate, as UIC levels of 250 ug/L and above are associated with an increase in subclinical hypothyroidism (Shi et al., 2015).
Fetal growth parameters are negatively affected by UIC <150 and >250 ug/L (i.e. Chen et al., 2018).
Data should have been stratified by WHO classifications:
- <150 Insufficient
150–249 Adequate
250–499 Above requirements [more-than-adequate]
≥500 Excessive
According to the study protocol, the mothers were asked to be fasting for 8 hours before study visits (Barman et al., 2018).
Research shows that fasting, especially early in the morning, may impact TSH levels (i.e. Nair et al., 2014).
Further adding to the confusion, drinking fluoride-laden water was allowed, as fasting for a blood test always excludes drinking water.
5. Season of Sampling
The study reports on the seasonal variations pertaining to urinary fluoride samples but made no effort to correlate with the seasonal variations of UIC and thyroid hormones (Kuzmenko et al., 2021).
SUMMARY
As reported by Aghaei et al. earlier (2015), this study found an increase in birth length with increasing fluoride intake. Many other previous studies have reported a decrease in birth weight with increasing fluoride intake.
Both iodine deficiency AND excess may affect birth weight and length. Both hypo- and hyperthyroidism are well-established to negatively affect birth outcomes, including LGA (Turunen et al., 2022; Dong et al., 2021).
Thyroid hormone controls fetal growth and development. Maternal thyroid hormones - upon which the fetus is dependent for the first 20 weeks - undergo drastic changes for the entire duration of gestation.
Maternal hypothyroxinemia has been found associated with LGA in numerous investigations (Li et al., 2021; Ovadia et al., 2022), while subclinical hypothyroidism is associated with SAG and lower birth weight (Derakhshan et al., 2020). Fluoride intake has been associated with both conditions.
Abnormal birth weight and length have also long been documented as a result of fluoride poisoning.
Likewise, the literature on the effects of fluoride on thyroid hormone metabolism now encompasses over 700 papers, dating back more than one hundred years. Over 280 studies have been published in the last twenty years alone.
The authors' conclusions that the effects of "gestational urinary fluoride concentrations" on birth length are not associated with thyroid hormones are not justified, as the authors conducted their investigation only late in pregnancy, while the effects would have likely occurred in the first half of gestation. In addition, a lack of knowledge and understanding of the effects of maternal iodine status/thyroid function contributed to a faulty model, resulting in an erroneous statistical evaluation.
PFPC Canada, August 2022
REFERENCES
Aghaei M, Derakhshani R, Raoof M, Dehghani M, Mahvi AH - "Effect of fluoride in drinking water on birth height and weight: an ecological study in Kerman Province, Zarand County, Iran" Fluoride 48:160-168 (2015)
https://www.researchgate.net/publicatio ... ounty_Iran

Chen R, Li Q, Cui W, Wang X, Gao Q, Zhong C, Sun G, Chen X, Xiong G, Yang X, Hao L, Yang N - "Maternal Iodine Insufficiency and Excess Are Associated with Adverse Effects on Fetal Growth: A Prospective Cohort Study in Wuhan, China" J Nutr 148(11):1814-1820 (2018)
https://pubmed.ncbi.nlm.nih.gov/30239801/
"The longitudinal analyses showed negative associations of maternal insufficient, more than adequate, or excessive iodine status with fetal growth during pregnancy (all P < 0.05)...Importantly, this study indicated that fetal FL in the second and third trimesters can be adversely affected by insufficient iodine status during early pregnancy."
de Escobar GM, Obregon MJ, del Rey FE - "Iodine deficiency and brain development in the first half of pregnancy" Public Health Nutr 10: 1554–1570 (2004)
Derakhshan A, Peeters RP, Taylor PN, Bliddal S, Carty DM, Meems M, Vaidya B, Chen L, Knight BA, Ghafoor F, Popova PV, Mosso L, Oken E, Suvanto E, Hisada A, Yoshinaga J, Brown SJ, Bassols J, Auvinen J, Bramer WM, López-Bermejo A, Dayan CM, French R, Boucai L, Vafeiadi M, Grineva EN, Pop VJM, Vrijkotte TG, Chatzi L, Sunyer J, Jiménez-Zabala A, Riaño I, Rebagliato M, Lu X, Pirzada A, Männistö T, Delles C, Feldt-Rasmussen U, Alexander EK, Nelson SM, Chaker L, Pearce EN, Guxens M, Steegers EAP, Walsh JP, Korevaar TIM - "Association of maternal thyroid function with birthweight: a systematic review and individual-participant data meta-analysis" Lancet Diabetes Endocrino 8(6):501-510 (2000) doi: 10.1016/S2213-8587(20)30061-9
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8168324/
"Maternal subclinical hypothyroidism in pregnancy is associated with a higher risk of SGA and lower birthweight, whereas isolated hypothyroxinaemia is associated with lower risk of SGA and higher birthweight. There was an inverse, dose-response association of maternal TSH and FT4 (even within the normal range) with birthweight."
Diouf M, Cisse D, Lo CM, Ly M, Faye D, Ndiaye O - "Pregnant women living in areas of endemic fluorosis in Senegal and low birthweight newborns: case-control study" Rev Epidemiol Sante Publique 60(2):103-8 (2012) French. doi: 10.1016/j.respe.2011.09.009
https://pubmed.ncbi.nlm.nih.gov/22424749/
"Low birthweight was associated with pregnant women living in endemic areas."
Dong J, Liu S, Wang L, Zhou X, Zhou Q, Liu C, Zhu J, Yuan W, Xu WY, Deng J - "Iodine monitoring models contribute to avoid adverse birth outcomes related more than adequate iodine intake" BMC Pregnancy Childbirth 21(1):454 (2021)
https://bmcpregnancychildbirth.biomedce ... 21-03936-w
"Multivariate logistic regression analysis showed that multivitamin supplements containing iodine and milk consumption were risk factors for more than adequate iodine (UIC ≥ 250 μg/L). Iodine-rich diet was significantly related to heavier birthweight, larger head circumference and longer femur length of the newborns while more than adequate iodine intake (UIC ≥ 250 μg/L) was a risk factor for macrosomia."
El Daouk M, Langer O, Lysikiewicz A - "First-trimester crown-rump length as a predictor of fetal LGA and SGA at term" J Matern Fetal Neonatal Med. 25(2):162-4 (2012). doi: 10.3109/14767058.2011.566653
"Mean first-trimester CRL of the 63 LGA-term neonates was 62.7 ± 6.0 mm (95% confidence interval, ± 1.49 mm; range, 61.21-64.19), while that of the 58 SGA-term neonates was smaller at 58.8 ± 6.9 mm (95% confidence interval, ± 1.79 mm; range, 57.01-60.59 mm). This 3.9 mm difference between the means was statistically significant (P = 0.01).
Conclusion: We found that birthweights of LGA and SGA neonates at term were associated with their first-trimester CRL measurements, thus, indicating that fetal growth patterns apparent early in pregnancy continue through term."
Gustin K, Barman M, Skröder H, Jacobsson B, Sandin A, Sandberg AS, Wold AE, Vahter M, Kippler M - "Thyroid hormones in relation to toxic metal exposure in pregnancy, and potential interactions with iodine and selenium" Environ Int 157:106869 (2021) doi: 10.1016/j.envint.2021.106869
https://pubmed.ncbi.nlm.nih.gov/34530290/
Gustin K, Barman M, Stråvik M, Levi M, Englund-Ögge L, Murray F, Jacobsson B, Sandberg AS, Sandin A, Wold AE, Vahter M, Kippler M - "Low-level maternal exposure to cadmium, lead, and mercury and birth outcomes in a Swedish prospective birth-cohort" Environ Pollut 265(Pt B):114986 (2020). doi: 10.1016/j.envpol.2020.114986
https://pubmed.ncbi.nlm.nih.gov/32585550/
"In multivariable-adjusted spline regression models, a doubling of maternal erythrocyte Cd (median: 0.29 μg/kg) above the spline knot of 0.50 μg/kg was associated with reduced birth weight (B: -191 g; 95% CI: -315, -68) and length (-0.67 cm; -1.2, -0.14). The association with birth weight remained when the analysis was restricted to never-smokers. Likewise, a doubling of erythrocyte Hg (median 1.5 μg/kg, mainly MeHg) above 1.0 μg/kg, was associated with decreased birth weight (-59 g; -115, -3.0), and length (-0.29 cm; -0.54, -0.047). Maternal Pb (median 11 μg/kg) was unrelated to birth weight and length. Erythrocyte Cd was primarily associated with intake of plant derived foods, Pb with game meat, tea and coffee, and Hg with fish. The results indicated that low-level maternal Cd and Hg exposure were associated with poorer birth anthropometry. Further prospective studies in low-level exposed populations are warranted."
Gustin K, Vahter M, Barman M, Jacobsson B, Skröder H, Filipsson Nyström H, Sandin A, Sandberg AS, Wold AE, Kippler M - "Assessment of Joint Impact of Iodine, Selenium, and Zinc Status on Women's Third-Trimester Plasma Thyroid Hormone Concentrations" J Nutr 152(7):1737-1746 (2022) doi: 10.1093/jn/nxac081
https://pubmed.ncbi.nlm.nih.gov/35383840/
SAME "NICE" COHORT.
"Results: Plasma zinc was most influential for all hormones but tT3, for which plasma selenium was most influential. In adjusted linear regression models, zinc was positively associated with tT4, tT3, and TSH, and <1200 μg/L also with fT4 and fT3. Selenium was inversely associated with fT3, and <85 μg/L with tT3."
Huang D, Zhu H, Zhu Y, Dang Q, Yang Q, Zhang Y, Cai X, Zhao X, Liang N, Wang H, Yu H - "Association of maternal HDL2-c concentration in the first trimester and the risk of large for gestational age birth" Lipids Health Dis 21(1):71 (2022) doi: 10.1186/s12944-022-01688-w.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9380360/
Kuzmenko NV, Tsyrlin VA, Pliss MG, Galagudza MM - "Seasonal variations in levels of human thyroid-stimulating hormone and thyroid hormones: a meta-analysis" Chronobiol Int 38(3):301-317 (2021) doi: 10.1080/07420528.2020.1865394
https://www.tandfonline.com/doi/abs/10. ... ode=icbi20
"We found that circulating TSH levels were higher in winter than in other seasons, and FT4 levels were higher in autumn than in winter. T4 level had no pronounced seasonal dynamics. The level of circulating T3 was significantly higher in winter than in summer and FT3 levels were lower in summer than in autumn and spring. In addition, analysis of TSH seasonal dynamics (winter vs summer) accounting for gender differences showed pronounced increases in TSH levels during winter in women, but not in men; and also significant increases in FT4 levels during summer in men, but not in women."
León G, Murcia M, Rebagliato M, Álvarez-Pedrerol M, Castilla AM, Basterrechea M, Iñiguez C, Fernández-Somoano A, Blarduni E, Foradada CM, Tardón A, Vioque J - "Maternal thyroid dysfunction during gestation, preterm delivery, and birthweight. The Infancia y Medio Ambiente Cohort, Spain" Paediatr Perinat Epidemiol 29(2):113-22 (2015). doi: 10.1111/ppe.12172
https://pubmed.ncbi.nlm.nih.gov/25565408/
"An inverse association of fT4 and TSH with birthweight was found, the former remaining when restricted to euthyroid women. High fT4 levels were also associated with an increased risk of SGA [odds ratio, 95% confidence interval (CI) 1.28 (95% CI 1.08, 1.51)]. Mean birthweight was higher in the hypothyroxinaemic group (β = 109, P < 0.01). Iodine intake and UIC were not associated with birth outcomes."
Li P, Cui J, Li L, Chen X, Ouyang L, Fan J, Lin S - "Association between isolated maternal hypothyroxinemia during the first trimester and adverse pregnancy outcomes in Southern Chinese women: a retrospective study of 7051 cases" BMC Pregnancy Childbirth 22(1):866 (2022) doi: 10.1186/s12884-022-05194-w
https://pubmed.ncbi.nlm.nih.gov/36424562/
"However, after using multivariate logistic regression analysis to adjust for confounders (maternal age, educational levels and preBMI), only LGA was shown to be associated with an increased risk in IMH women [adjusted OR: 1.27 (95% CI 1.044-1.566)]."
Margetaki K, Vafeiadi M, Kampouri M, Roumeliotaki T, Karakosta P, Daraki V, Kogevinas M, Hu H, Kippler M, Chatzi L - "Associations of exposure to cadmium, antimony, lead and their mixture with gestational thyroid homeostasis" Environ Pollut 289:117905 (2021) doi: 10.1016/j.envpol.2021.117905
https://pubmed.ncbi.nlm.nih.gov/34371266/
"In addition, women with high urinary Cd had 2.2 % (95%CI: 0.0 %, 4.4 %) higher fT4 and 4.0 % (95%CI: -0.1 %, 8.1 %) higher fT3 levels, and women with high urinary Pb had 4 % (95%CI: 0.2 %, 8.0 %) higher fT3 levels compared to women with low exposure. The negative association of Cd with TSH persisted only when iodine sufficiency was unfavorable. BKMR attested that simultaneous exposure to toxic metals was associated with decreased TSH and increased fT3 and revealed a potential synergistic interaction of Cd and Pb in association with TSH. The present results suggest that exposure to toxic metals even at low levels can alter gestational thyroid homeostasis."
Männistö T, Vääräsmäki M, Pouta A, Hartikainen AL, Ruokonen A, Surcel HM, Bloigu A, Järvelin MR, Suvanto-Luukkonen E - "Perinatal outcome of children born to mothers with thyroid dysfunction or antibodies: a prospective population-based cohort study" J Clin Endocrinol Metab 94(3):772-9 (2009)doi: 10.1210/jc.2008-1520
https://pubmed.ncbi.nlm.nih.gov/19106271/
"The offspring of TPO-Ab- and TG-Ab-positive mothers had higher perinatal mortality, which was not affected by thyroid hormone status. Unadjusted and adjusted (for maternal age and parity) risk for increased perinatal mortality was an odds ratio of 3.1 (95% confidence interval 1.4-7.1) and 3.2 (1.4-7.1) in TPO-Ab- and 2.6 (1.1-6.2) and 2.5 (1.1-5.9) in TG-Ab-positive mothers. TPO-Ab-positive mothers had more large-for-gestational age infants (2.4 vs. 0.8%, P = 0.017), as did mothers with low TSH and high fT4 concentrations vs. reference group (6.6 vs. 2.5%, P = 0.045). Significantly higher placental weights were observed among mothers with low TSH and high fT4 or high TSH and low fT4 levels as well as among TPO-Ab-positive mothers....Conclusions: First-trimester antibody positivity is a risk factor for perinatal death but not thyroid hormone status as such. Thyroid dysfunction early in pregnancy seems to affect fetal and placental growth."
Medici M, Ghassabian A, Visser W, de Muinck Keizer-Schrama SM, Jaddoe VW, Visser WE, Hooijkaas H, Hofman A, Steegers EA, Bongers-Schokking JJ - "Women with high early pregnancy urinary iodine levels have an increased risk of hyperthyroid newborns: the population-based Generation R Study"
Clin Endocrinol (Oxf) 80:598-606 (2014)
Nair R, Mahadevan S, Muralidharan RS, Madhavan S - "Does fasting or postprandial state affect thyroid function testing?" Indian J Endocrinol Metab. 18(5):705-7 (2014) doi: 10.4103/2230-8210.139237
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4171896/
"TSH was suppressed in all subjects after food irrespective of the fasting levels. Free T4 values did not change significantly. This resulted in reclassification of 15 out of 20 (75%) subjects as subclinical hypothyroidism (SCH) based on fasting values whose TSH values were otherwise within range in the postprandial sample. This may have an impact on the diagnosis and management of hypothyroidism especially where even marginal changes in TSH may be clinically relevant as in SCH and in pregnancy."
Ortíz-García SG, Torres-Sánchez LE, Muñoz-Rocha TV, Mercado-García A, Peterson KE, Hu H, Osorio-Yáñez C, Téllez-Rojo MM - "Maternal urinary fluoride during pregnancy and birth weight and length: Results from ELEMENT cohort study" Sci Total Environ 838(Pt 3):156459 (2022). doi: 10.1016/j.scitotenv.2022.156459
https://www.sciencedirect.com/science/a ... via%3Dihub
Papastefanou I, Souka AP, Pilalis A, Eleftheriades M, Michalitsi V, Kassanos D - "First trimester prediction of small- and large-for-gestation neonates by an integrated model incorporating ultrasound parameters, biochemical indices and maternal characteristics" Acta Obstet Gynecol Scand 91(1):104-111 (2012) doi: 10.1111/j.1600-0412.2011.01271.x
https://pubmed.ncbi.nlm.nih.gov/21895614/
"Prediction for birthweight deviations is feasible using data available at the routine 11-14 weeks' examination."
PFPC - "Cadmiosis = Fluorosis" (2013)
viewtopic.php?f=29&t=680
Stråvik M, Gustin K, Barman M, Skröder H, Sandin A, Wold AE, Sandberg AS, Kippler M, Vahter M - "Infant Iodine and Selenium Status in Relation to Maternal Status and Diet During Pregnancy and Lactation" Front Nutr 8:733602 (2021). doi: 10.3389/fnut.2021.733602. PMID: 34988107; PMCID: PMC8721874.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8721874/
Turunen S, Vääräsmäki M, Marttila R, Leinonen MK, Gissler M, Männistö T, Suvanto E - "Indications for intensive care unit treatment among neonates born to mothers with thyroid disease: A population-based cohort study" Acta Obstet Gynecol Scand 101(10):1093-1101 (2022) doi: 10.1111/aogs.14413
https://pubmed.ncbi.nlm.nih.gov/35778835/
"The preterm neonates, neonates with low birthweight, and large-for-gestational-age infants had increased odds of NICU admission if their mother had hypothyroidism. Also neonates with cardiovascular problems, jaundice or hypoglycemia associated with maternal diabetes had increased odds of NICU admissions if their mother had hypothyroidism. Further, the preterm neonates, large-for-gestational-age infants, and term infants with jaundice had increased odds of NICU admission if their mother had hyperthyroidism."
Young AE, Kemp JF, Uhlson C, Westcott JL, Ali SA, Saleem S, Garcès A, Figueroa L, Somannavar MS, Goudar SS, Hambidge KM, Hendricks AE, Krebs NF; Women First Preconception Maternal Nutrition Trial Group - "Improved first trimester maternal iodine status with preconception supplementation: The Women First Trial" Matern Child Nutr 17(4):e13204 (2021). doi: 10.1111/mcn.13204
"Nominally significant positive associations were observed between I/Cr at 12 weeks and birth length and head circumference z-scores (p = 0.028 and p = 0.005, respectively)."
Zhu YD, Han Y, Huang K, Zhu BB, Yan SQ, Ge X, Zhou SS, Xu YY, Ren LI, Sheng J, Pan WJ, Hao JH, Zhu P, Tao FB - "The impact of isolated maternal hypothyroxinaemia on the incidence of large-for-gestational-age infants: the Ma'anshan Birth Cohort study" BJOG 125(9):1118-1125 (2018) doi: 10.1111/1471-0528.15107
First T: (mean = 10.01 weeks; SD 2.13) 2nd T: (mean = 25.64 weeks; SD 1.07)
"However, an increased risk of LGA was observed among IMH women in the second trimester (OR: 2.088, 95% CI: 1.193-3.654). Maternal TPO-Ab positivity in the second trimester increased the risk of SGA (OR: 2.094, 95% CI: 1.333-3.290)."
Last edited by wendy on Fri Feb 24, 2023 3:43 am, edited 6 times in total.
-
admin
- Site Admin
- Posts: 6757
- Joined: Tue Jan 18, 2005 10:25 pm
Re: 2022 - Sweden NICE - Birth weight and fluoride | Thyroid
NOTE: Interestingly, a recent study investigating the effects of PFAS (organic fluoride compounds) on birth - involving Grandjean - also claimed that thyroid hormones "were not found to mediate associations between PFASs and birth size."
In that particular study, thyroid hormones were not investigated until 34 weeks of gestation! (Xiao et al., 2022)
Xiao C, Grandjean P, Valvi D, Nielsen F, Jensen TK, Weihe P, Oulhote Y - "Associations of Exposure to Perfluoroalkyl Substances With Thyroid Hormone Concentrations and Birth Size" J Clin Endocrinol Metab. 105(3):735–45 (2020). doi: 10.1210/clinem/dgz147
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7112969/
"Several PFASs were negatively associated with birth weight, length, and head circumference, and a general positive association between maternal serum-PFASs and cord serum-thyroid-stimulating hormone (TSH; also known as thyrotropin) was found. For instance, a doubling in perfluorooctane sulfonate (PFOS) and perfluorooctanoic acid (PFOA) was associated with a 53% (95% CI, 18%-99%) and 40% (95% CI, 8%-81%) increases in TSH concentrations, respectively. There was little evidence of sexually dimorphic associations. Overall, THs were not found to mediate associations between PFASs and birth size.
Conclusion: In this study, several PFASs were negatively associated with birth size and increased THs; however, this did not explain lower birth weight among children exposed to PFAS."
In that particular study, thyroid hormones were not investigated until 34 weeks of gestation! (Xiao et al., 2022)
Xiao C, Grandjean P, Valvi D, Nielsen F, Jensen TK, Weihe P, Oulhote Y - "Associations of Exposure to Perfluoroalkyl Substances With Thyroid Hormone Concentrations and Birth Size" J Clin Endocrinol Metab. 105(3):735–45 (2020). doi: 10.1210/clinem/dgz147
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7112969/
"Several PFASs were negatively associated with birth weight, length, and head circumference, and a general positive association between maternal serum-PFASs and cord serum-thyroid-stimulating hormone (TSH; also known as thyrotropin) was found. For instance, a doubling in perfluorooctane sulfonate (PFOS) and perfluorooctanoic acid (PFOA) was associated with a 53% (95% CI, 18%-99%) and 40% (95% CI, 8%-81%) increases in TSH concentrations, respectively. There was little evidence of sexually dimorphic associations. Overall, THs were not found to mediate associations between PFASs and birth size.
Conclusion: In this study, several PFASs were negatively associated with birth size and increased THs; however, this did not explain lower birth weight among children exposed to PFAS."